Total Knee Joint Replacement
Total Knee Joint Replacement
R.N H Hospital Pvt Ltd recognized this long ago and today it is a leading tertiary referral trauma center in central india.

Knee anatomy
The knee is the most complex joint in the human body..
The knee is a hinge joint that is responsible for weight-bearing and movement. It consists of bones, meniscus, ligaments, and tendons.
The knee is designed to fulfill a number of functions:
- Support The Body In An Upright Position Without The Need For Muscles To Work
- Helps To Lower And Raise The Body
- Provides Stability
- Acts As A Shock Absorber
- Allows Twisting Of The Leg
- Makes Walking More Efficient
- Helps Propel The Body Forward
Below, we will explain the basic components of knee anatomy.

Bones
The femur (thigh bone), tibia (shin bone), and patella (kneecap) make up the bones of the knee. The knee joint keeps these bones in place.
The patella is a small, triangle shaped bone that sits at the front of the knee, within the quadriceps muscle. It is lined with the thickest layer of cartilage in the body because it endures a great deal of force.

Ligaments
Ligaments are tough and fibrous tissues; they act like strong ropes to connect bones to other bones, preventing too much motion and promoting stability. The knee has four:
- ACL (anterior cruciate ligament) – prevents the femur from sliding backward on the tibia, and the tibia from sliding forward on the femur.
- PCL (posterior cruciate ligament) – prevents the femur from sliding forward on the tibia, or the tibia from sliding backward on the femur.
- MCL (medial collateral ligament) – prevents side to side movement of the femur.
- LCL (lateral collateral ligament) – prevents side to side movement of the femur.

Muscles
Although they are not technically part of the knee joint, the hamstrings and quadriceps are the muscles that strengthen the leg and help flex the knee.
The quadriceps are four muscles that straighten the knee. The hamstrings are three muscles at the back of the thigh that bend the knee.
The gluteal muscles – gluteus medius and minimus – also known as the glutes are in the buttocks; these are also important in positioning the knee.
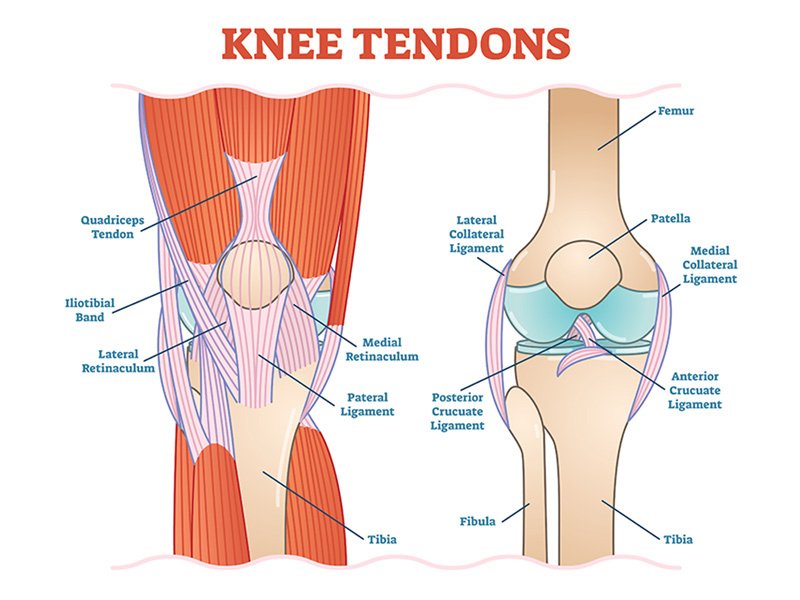
Tendons
These tough bands of soft tissue provide stability to the joint. They are similar to ligaments, but instead of linking bone to bone, they connect bone to muscle. The largest tendon in the knee is the patellar tendon, which covers the kneecap, runs up the thigh, and attaches to the quadriceps.

Joint capsule
The joint capsule is a membrane bag that surrounds the knee joint. It is filled with a liquid called synovial fluid, which lubricates and nourishes the joint.

Bursa
There are approximately 14 of these small fluid-filled sacs within the knee joint. They reduce friction between the tissues of the knee and prevent inflammation.
 CARTILAGE
CARTILAGE
There are two types of cartilage in the knee :

Meniscus
These are crescent-shaped discs that act as a cushion, or “shock absorber” so that the bones of the knee can move through their range of motion without rubbing directly against each other. The menisci also contain nerves that help improve balance and stability and ensure the correct weight distribution between the femur and tibia.
The knee has two menisci :
- Medial – on the inner side of the knee, this is largest of the two
- Lateral – on the outer side of the knee

Articular cartilage
Found on the femur, the top of the tibia, and the back of the patella; it is a thin, shiny layer of cartilage. It acts as a shock absorber and helps bones move smoothly over one another.
 WHAT IS KNEE JOINT REPLACEMENT ?
WHAT IS KNEE JOINT REPLACEMENT ?

Knee joint replacement is a procedure that involves replacing an injured or ailing knee with an artificial joint, or prosthesis.
The prosthesis is made of metal alloys, plastics, and polymers. It mimics the function of a knee. According to the American Academy of Orthopaedic Surgeons (AAOS), replacement knees can fit your needs and specifications.
When selecting a prosthetic knee, your doctor will take into account your :

AGE

WEIGHT

ACTIVITY LEVEL

OVERALL HEALTH
The procedure to remove your old knee and replace it with a prosthesis usually takes less than two hours, but recovery and rehabilitation can last months.
Another name for this procedure is knee arthroplasty. Knee replacements are a very common surgery.
 WHAT IS THE PURPOSE OF A KNEE JOINT REPLACEMENT ?
WHAT IS THE PURPOSE OF A KNEE JOINT REPLACEMENT ?

Damage from arthritis is the most common reason for knee joint replacement. This includes both osteoarthritis and rheumatoid arthritis. Doctors usually only recommend knee replacement after other, less invasive treatments have failed. First-line treatment options include:
- Weight loss
- Medications
- Physical therapy
- Assistive devices, such as a cane or a knee brace

Key factors in determining if you’re a good candidate for knee joint replacement include :
- how much your knee pain interferes with daily activities, such as walking or climbing stairs
- if your knee is deformed, bows, or “blows out” regularly
- your age
- your overall health
Knee surgery is a typical treatment for people over the age of 55. Younger people who have their knees replaced may outlive their artificial knees and may need a revision.
Doctors evaluate each candidate for knee replacement surgery on an individual basis.
 HOW DO YOU PREPARE FOR KNEE JOINT REPLACEMENT ?
HOW DO YOU PREPARE FOR KNEE JOINT REPLACEMENT ?
Before surgery, your doctor will assess your overall health and anesthesia risks. This evaluation will include:

A FULL MEDICAL HISTORY

A PHYSICAL EXAMINATION

BLOOD TESTS

X-RAYS

OTHER IMAGING TESTS

Your doctor will ask you for your complete medical history, including any prior surgeries and ongoing health conditions you have. Tell your doctor about any medication you’re taking including over-the-counter medicines and nutritional supplements. You may have to stop taking some or all of them before your surgery.
Also, tell your doctor if you’ve ever had an allergic reaction to anesthesia. Your doctor will review your anesthesia options based on your preferences and what they think is appropriate for your situation. This could include general anesthesia, which means you’re asleep during surgery. Or, you may receive anesthesia in your spine, which leaves you awake but pain-free from the waist down.
Your doctor will give your surgeon the results of your medical evaluation, medical history, and your anesthesia choice.
You can expect to walk with the aid of crutches or a walker for several weeks. Before surgery, you should prepare your home to accommodate your recovery :
- You May Need To Install Handles In Showers And Around The Toilet.
- It’s Good To Have A Chair And Footrest Available So You Can Elevate Your Leg.
- If Possible, Keep Your Living Space On The First Floor If You Have A Multistory House.
Your doctor and surgical team will give you full instructions on how to best prepare for surgery. It’s important to follow those instructions as closely as possible.

 WHAT HAPPENS DURING KNEE JOINT REPLACEMENT ?
WHAT HAPPENS DURING KNEE JOINT REPLACEMENT ?

When it’s time for your surgery, you’ll change into a hospital gown and get an IV to provide you with fluids and nutrients during the surgery. Just before surgery, you’ll receive anesthesia.
During the procedure, which lasts between one and two hours, your surgeon will make a long surgical cut above your knee. With the skin and muscle pulled back, they’ll cut away damaged cartilage and bone.
They’ll affix the new knee joint to your femur, or thighbone, and tibia, which is the main bone in your lower leg. They’ll do this using specialized cement, pins, and screws. Afterward, your surgeon will close the incision wound with stitches and apply a bandage.
You’ll recover from the surgery in a special recovery room where a team can monitor your vital signs.
 WHAT HAPPENS AFTER KNEE JOINT REPLACEMENT ?
WHAT HAPPENS AFTER KNEE JOINT REPLACEMENT ?
After surgery, your leg will feel stiff. You’ll experience some pain. Receiving painkillers through your vein, or intravenously, can help manage this pain. You may receive long-acting local anesthetics at the time of surgery or possibly a nerve block to help with postoperative pain. You’ll also receive medication to prevent your blood from clotting.
Most people begin physical therapy the day of surgery or day after their surgery to promote blood flow to the tissues around the new knee. Your surgeon may recommend using a continuous passive-motion machine. This is a special brace-like device that continuously moves your knee in a gentle bending motion.
Your surgeon will let you know when it’s best to leave the hospital. This is based on the results of the surgery and your condition.
Following your surgery, you’ll undergo considerable physical therapy. Your surgeon and physical therapy team will design a program that’s right for you.

